REVISIÓN |
Dry eye disease compounds currently under evaluation in clinical trials
Basilio Colligris, Jesús Pintor*
Departamento de Bioquímica y Biología Molecular IV, Facultad de Óptica y Optometría, Universidad Complutense de Madrid, Madrid, España.
*e-mail: jpintor@vet.ucm.es
Recibido el 31 de marzo de 2014 - An. Real Acad. Farm. Vol 80, Nº 1(2014), pág. 151-178
ABSTRACT
Dry eye syndrome is a common disorder provoking changes in tear quantity and composition being the most common ophthalmic manifestation of systemic inflammatory diseases. Untreated dry eye could cause increased risk of ocular infection, corneal ulcer and blindness. Only a few drugs are authorized so far for the treatment of dry eye disease and the possibilities of evolution in this sector are immense. Accordingly, the future tendency is towards the development of drugs to control the inflammation or stimulate the mucin and tear secretion. A significant number of new potential solutions are under development or placed in the pharmaceutical pipeline, promising better results and lesser side effects, but still leaving unattended the main causes of the disease. In this article, we review the corresponding literature, recent clinical trials data and patents concerning future pharmaceutical compounds for dry eye disease treatment, presenting the new strategic movements of the pharmaceutical industry. |
Keywords: Dry eye; anti-inflammatory; keratoconjunctivitis sicca; keratitis sicca; xerophthalmia; mucin secretion; tear secretion; NSAID.
RESUMEN
Fármacos de la enfermedad de ojo seco actualmente en evaluación en ensayos clínicos
El síndrome de ojo seco es un trastorno bastante común, que provoca cambios en la cantidad y la composición de la lágrima, siendo la manifestación oftálmica más común de enfermedades inflamatorias sistémicas. El ojo seco no tratado puede provocar un aumento del riesgo de infección ocular, úlceras corneales y en casos extremos ceguera. Actualmente sólo unos pocos fármacos están autorizados para el tratamiento de la enfermedad y las posibilidades de evolución en este sector son inmensas. La tendencia del futuro está dirigida hacia el desarrollo de fármacos que controlan la inflamación o estimulan la secreción de las mucinas y del componente acuoso de las lágrimas. Un número significativo de nuevos compuestos están en desarrollo o ya están en ensayos clínicos, con aparentes mejores resultados y efectos secundarios menos adversos, pero una vez más dejando desatendidas las principales causas de la enfermedad. En este artículo revisamos la literatura correspondiente, los últimos datos de los ensayos clínicos y las patentes relativas a futuros compuestos farmacéuticos para el tratamiento de la enfermedad del ojo seco, desvelando los nuevos movimientos estratégicos de la industria farmacéutica. |
Palabras clave: Ojo seco, anti-inflamatorios, queratoconjuntivitis sicca, queratitis seca, xeroftalmia, secreción de mucinas; secreción de lágrima; antiinflamatorios no esteroideos.
introductIon
Dry eye disease is a chronic ocular disorder affecting approximately 10-20% of the population worldwide, being relatively frequent among women especially after the menopause (1, 2). This pathology is closely related to the aging and it is progressively affecting larger parts of the population. Almost everyone experiences ocular irritation or the symptoms of dry eye under certain conditions, such as prolonged working on a computer, being in a dry environment or after using certain drugs (3-5). Patients with autoimmune diseases are prone to suffer from dry eye inflammation, which is a key factor in the onset of severe dry eye disease (6).
The pathology occurs when the ocular surface tear protective layer is weakened which could be the result of insufficient or atypical production of one or more tear components (7). Tear film forms a moist natural barrier separating eye from the external media. This consistent film is formed mainly from a triplet of aqueous, mucous, and lipid layers providing the necessary equilibrium for the healthy maintenance of the ocular surface (Figure 1). The main functions of this film are: lubrication of the ocular surface, transfer of nutritional elements to the cornea, elimination of foreign matter and cellular debris generated on the ocular surface by the tear flow and the blink process, and acting as the first line of defense against ocular surface infections (8). In some cases, the imbalance of the tear film composite layers leads to reduced tear secretion, exposure of the eye surface, dryness and damage of the surface cells (6). The imbalance of the composite layers could be caused by Sjögren’s syndrome tear secretion deficiency and/or tear film instability due to the use of contact lenses (6, 9, 10). Dry eye syndrome types are classified according to etiologic perspectives and environmental influences as: aqueous deficient dry eye (ADDE) and evaporative-tear dry eye (EDE) (6, 11). ADDE is divided to: related to Sjögren’s syndrome (primary and secondary) and non-related to Sjögren’s syndrome conditions (lacrimal disease, lacrimal obstruction and malfunctioning blinking reflex) (6). EDE conditions are: oil deficient, lid related and caused by an ocular surface alteration (6). Signs and symptoms of these complications can vary from patient to patient, sometimes with little or no correlation between them, even though they are generally related to the tear film composition. The signs and symptoms could include keratitis, conjunctival and corneal staining, redness, blurry vision, decreased tear film break-up time, decreased tear production, volume, and flow, increased conjunctival redness, excess debris in the tear film, ocular dryness, ocular grittiness, ocular burning, foreign body sensation in the eye, excess tearing, photophobia, ocular stinging, refractive impairment, ocular sensitivity, and ocular irritation (12, 13).
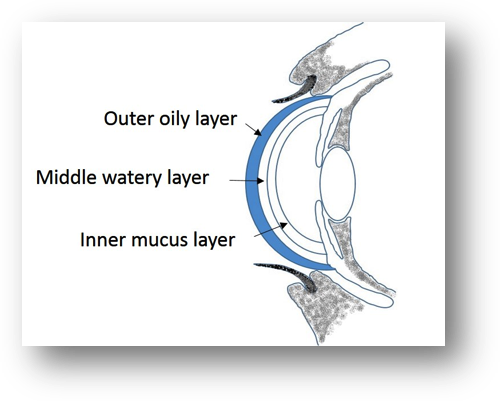
Figure 1.- Tear film layers. |
Currently there are only a few pharmaceutical treatments for dry eye. In some countries like Japan, are commercialized more DED treatment drugs than in Europe and the USA as the approval rules are not so rigorous. Another important factor concerning DED treatment is that in most of the cases, the biotechnology companies are trying to sort out the problem based on “over the counter” strategies, trying to relieve symptoms rather than getting to the cause of the disease. Consequently, for the symptomatic relief of dry eye we could mention the following treatments currently used: Supplements called “artificial tears” which are synthetic lubricants, characterized by hypotonic or isotonic buffered solutions containing electrolytes, surfactants and several types of viscosity agents (17). The “artificial tears” permit not only the increase of tear quantity, but also to keep the ocular surface moistened and relieve discomfort. Another type of treatment is the tear retention devices/implants also known as punctal plugs. They have been developed to occlude the lacrimal puncta and they can be absorbable and non-absorbable (18). These devices keep tears longer on the ocular surface relieving the patient’s from the undesirable symptoms. Other type of treatment is the moisture chamber spectacles. It has been reported that increased periocular humidity can cause the tear film lipid layer to thicken and that spectacle wearers with dry eye have a longer inter-blink interval than the non-spectacle wearers (19). Current treatments are mainly focused on addressing inflammation and tear restoration (20). Dry eye disease is the outcome of many factors resulting in inflammation of cornea and conjunctiva. The dysfunction of the tear secretory glands leads to changes in tear composition such as hyper-osmolarity which stimulates the production of inflammatory mediators on the ocular surface. This inflammation can be initiated either by chronic irritative stress like wearing contact lens wearing or from a systemic inflammatory autoimmune disease like rheumatoid arthritis (21, 22). Anti-inflammatory drugs are widely used for the treatment of the inflammation produced by diseases. Topical corticosteroids can relieve moderate or severe dry eye symptoms and signs rapidly and effectively (23). Steroids on the other hand may cause severe side effects after prolonged use. The undesired effects vary from bacterial or fungal infection, elevated intraocular pressure and cataract formation. Additionally, steroids suppress locally the immune response in patients with already compromised ocular surface. Therefore, steroids are typically used only for a limited period of time in dry eye patients (20). Due to the above-mentioned reasons, non-steroidal anti-inflammatory drugs (NSAID) credited as causing less severe side effects are recently evaluated as a potential dry eye treatment. The NSAIDs could decrease inflammation and eye discomfort due to their analgesic effect, but they might induce DED decreasing sensitivity. In 2002 U.S. Food and Drug Administration (FDA) approved the drug RESTASIS® of the company Allergan as the first prescription medicine capable to increase tear production (24). Topical RESTASIS® is an ophthalmic emulsion containing cyclosporine 0.05%. Other types of drug used are the antibiotics like azithromycin, and tetracycline. Furthermore, some research groups are studying the use of serum tears and the intense pulse light as potential treatments (20). On the following pages, we present some future treatments currently passing clinical trials.
AL-2178/Rimexolone
AL-2178/Rimexolone 1% (Figure 2) is a glucocorticoid steroid developed by Alcon, as a treatment for dry eye disease. Rimexolone inhibits T-cell proliferation as well as cytokine production of activated CD4+ T-cells in a similar manner to dexamethasone (25). The compound passed successfully from Phase III clinical trials (ClinicalTrials.gov Identifier: NCT00471419) in May 2007 and now is marketed as a 1% eye drop suspension under the trade name Vexol by Alcon Laboratories (26).
LX214/Voclosporin
LX214-voclosporin (Figure 3) is an immunosuppressant drug developed by Isotechnika and Lux Biosciences. Voclosporin is a calcineurin inhibitor, analog of cyclosporin with enhanced action against calcineurin and a greater metabolic stability. It is already used as a treatment of various forms of non-infectious uveitis (27). The two companies are evaluating voclosporin ophthalmic solution as a treatment for dry eye disease in a Phase I clinical trial (ClinicalTrials.gov Identifier: NCT00851734), but did not publish results over its efficacy (28).
Tofacitinib
Pfizer Inc. developed a JAK inhibitor called Tofacitinib (formerly CP-690550 - Tasocitinib) (Figure 4) capable to interfere the JAK-STAT signaling pathway, which transmits extracellular information into the cell nucleus, influencing DNA transcription (29). The company concluded phase I/II trials (ClinicalTrials.gov Identifier: NCT00784719) in patients for various disorders including dry eye disease. The trials demonstrated improvement in the signs and symptoms on dry eye patients and the use of the drug was well tolerated and without severe side effects (30). Huang and colleagues conducted a study to 82 patients with moderate to severe dry eye disease, treated for eight weeks with 0.0001% to 0.005% tofacitinib once or twice daily. The patients showed reduction in conjunctival cell surface HLA-DR expression, tear levels of pro-inflammatory cytokines and inflammation markers. The markers in tears included MMP-9, IL-15, IL-17A, and IL-12p70 (31).
Nutrilarm®-Omega-3 and Omega 6 fatty acids-T1675
Omega-3 and omega-6 essential fatty acids (EFA) are the origin of a family of compounds called eicosanoids. Eicosanoids are signaling molecules produced by the oxidation of 20-carbon fatty acids and they are mediators of various inflammatory processes. In general, the omega-3 derived compounds, systemic linoleic (LA) and gamma-linolenic acid (GLA) are reducing eye inflammation, and n-6 pathway eicosanoids are considered as promoting inflammation (32, 33). Omega-3 and omega-6 EFAs are used for dry eye treatment due to their anti-inflammatory effects such as the drug Nutrilarm® of the French company Théa Laboratoires, which is already commercialized in Europe. This medicine uses a supplementation of omega-3 and omega-6 fatty acids, which according to the company reduce expression of the conjunctival inflammatory marker human leucocyte antigen-DR (HLA-DR) and may help improving DED symptoms. The compound past in 2006 from Phase II clinical trials in US (ClinicalTrials.gov Identifier: NCT00357201) but the company decided to continue the pre-clinical development to resolve efficacy and doses issues (34-36).
Oral Omega-3-acid ethylesters
Pennsylvania State University and the American Society of Cataract and Refractive Surgery Foundation (ClinicalTrials.gov Identifier: NCT01107964) started in April 2010 a clinical study, based on the hypothesis that oral omega-3-acid ethyl esters (Lovaza, GlaxoSmithKline) will decrease the dry-eye related symptoms as well as clinical markers associated to dry eye disease. The preliminary results of the study are positive but more research is needed to define the composition and dosing of the treatment. From the results it was confirmed the relationship between EFA supplementation and improvement in dry eye symptoms in patients (37). Nevertheless before any anti-inflammatory therapy is necessary a detailed examination of a patient due to the complexity of the disease and to provide individual and successful treatment (38).
Secukinumab and Canakinumab
Novartis Pharmaceuticals Inc. presented two novel antibodies, Secukinumab (AIN457) and Canakinumab (ACZ885). Secukinumab is a fully human monoclonal antibody designed to bind selectively, inhibiting the member A of interleukin 17cytokine family, a key driver of immune-mediated diseases. Canakinumab is a fully human monoclonal antibody, inhibiting solely interleukin 1β (IL-1β), the form of the interleukin-1 protein that is the main cause of various inflammatory diseases (39). Currently both antibodies are under development as treatments of a wide range of auto inflammatory diseases. In November 2010 Novartis started a Phase II study on effects of a single intravenous administration of Secukinumab 10 mg/kg or Canakinumab 10 mg/kg on 72 dry eye patients (ClinicalTrials.gov Identifier: NCT01250171). The study reports suggest that both substances are well tolerated in most patients, and no serious adverse effects have been reported. The drugs provide significant advantages over existing competitive therapies, including bimonthly administration and an approved use in children (40-42).
MIM-D3
Mimetogen Pharmaceuticals Inc. is developing MIM-D3, a small molecule mimicking the nerve growth factor (NGF) activity (Figure 5). NGF stimulates the conjunctival cell glycoconjugate secretion and during in vivo trials demonstrated therapeutic efficacy on dry eye disease (43). NGF plays an important role in ocular surface maintenance, corneal wound healing, displaying a mucin secretagogue activity in conjunctival cells (44). Jain and colleagues during evaluation studies demonstrated that a 1% MIM-D3 dose increased glycoconjugate concentration, improving the quality and stability of tear film and the healing on the ocular surface in dry eye (45). Mimetogen conducted Phase II safety and efficacy studies (ClinicalTrials.gov Identifier: NCT01257607) from December 2010 to October 2012, on 150 patients with the application of 1% MIM-D3 and 5% MIM-D3 for 28 days. Unfortunately the target primary endpoints were not met completely. Despite this negative development the company continues the development considering MIM-D3 as a potent compound (46).
Difluprednate
Alcon is evaluating the corticosteroid Difluprednate-Durezol, a butyrate ester of 6(alpha),9(alpha)-difluoro prednisolone acetate as a potential treatment for dry eye disease (Figure 6) (47). This corticosteroid is preventing the phospholipid release and decreases the eosinophil action. Durezol received approval from the FDA in 2008 as the first ophthalmic steroid for the postoperative inflammation and pain. Alcon started clinical trials Phase II (ClinicalTrials.gov Identifier: NCT01276223) in January 2011 for the Difluprednate ophthalmic emulsion 0.05%, one drop in each eye twice per day, on 726 patients, as an anti-inflammatory treatment of dry eye disease. Mulki and colleagues are suggesting that difluprednate 0.05% ophthalmic emulsion exhibits enhanced penetration, decent bioavailability, rapid local metabolism and strong efficacy, with a low incidence of adverse effects and a comparable safety profile (48).
Cis-urocanic acid
LaurantisPharma Ltd and Kuopio University Hospital are developing eye drops containing Cis-urocanic acid (cis-UCA) as treatment for ocular surface inflammation associated with moderate to severe dry eye syndrome. Cis-urocanic acid inhibits the SAPK/JNK signaling pathway in ultraviolet B (UV-B) exposed human corneal epithelial cells in vitro, having important implications in the management of inflammatory eye conditions since chronic stress is directly linked to cytotoxicity in epithelial cells. During tests it was demonstrated that is inhibiting the secretion of pro-inflammatory cytokines from human conjunctival and corneal epithelial cells after UV-B-induced stress reaction (49, 50). Preclinical studies in relevant animal models of eye inflammation also demonstrated that cis-UCA may be a safer and more effective alternative to current drugs used for acute and long-term treatment of dry eye. From November 2011 to May 2012 Laurantis conducted Phase I (ClinicalTrials.gov Identifier: NCT01476332), safety, tolerability and pharmacokinetics studies of 0.5% and 2.5% Cis-UCA eye drops in adult healthy volunteers. The results are not published, but the company continues the development of the compound.
Thymosin Beta 4
RegeneRx Biopharmaceuticals is developing RGN-259 which is a 0.1% Thymosin Beta 4 (Tβ4) ophthalmic solution as a novel therapeutic treatment for dry eye (51, 52). Thymosin Beta 4 is a synthetic version of a naturally occurring peptide, used clinically as a tissue repair and regeneration peptide (53). In human body is a protein encoded by the TMSB4X gene (GenBank accession number: NC_000023.10). During preclinical evaluations it was demonstrated that Tβ4 is promoting corneal epithelial intercellular adhesions following injury in animal models of dry eye (54). In June 2011 RegeneRx started Phase II safety and efficacy studies (ClinicalTrials.gov Identifier: NCT01387347) of the RGN-259 ophthalmic solution in patients with dry eye syndrome. The study has been completed in December 2012 and in ARVO 2012 the company presented the results, claiming the statistically significant reduction in central corneal fluorescein staining from baseline compared to placebo and also a greater reduction in exacerbation of ocular discomfort (55).
Belimumab
Belimumab is a human monoclonal antibody inhibiting B-cell activating factor (BAFF) and is developed by the University of Udine as a treatment for Sjögren’s syndrome. Sjögren's syndrome is a systemic autoimmune disease characterized by an increase in BAFF (BLyS) levels resulting in B cell hyperactivity. B cells are involved in the pathogenesis of SS in both systemic and glandular features, and B cell down regulation may lead to a decrease of disease activity. Moreover, pathogenesis of SS is closed to that of systemic lupus erythematosus, where belimumab has been proven to be effective. Currently the compound is under Phase II clinical trials evaluation (ClinicalTrials.gov Identifier: NCT01160666) and the initial results are promising (56).
Rituximab
Rituximab (CD20) is developed by IDEC Pharmaceuticals as a treatment for Sjögren’s syndrome. CD20 antigen is targeting cells of the B-cell lineage, leading to transient blood B-cell depletion, leaving aside stem cells (57). Rituximab is already approved by the U.S. Food and Drug Administration in 1997 as a treatment of B-cell non-Hodgkin lymphomas resistant to other chemotherapy regimens. The compound currently is tested in Phase III clinical trials (ClinicalTrials.gov Identifier: NCT00740948) to study the tolerance and efficacy of rituximab injection in Sjögren’s disease (58, 59).
Lotemax
Bausch & Lomb, Inc. is re-purposing the already approved drug Lotemax with topical cyclosporine ophthalmic emulsion 0.05% (Restasis) as a possible treatment of dry eye. Lotemax (loteprednoletabonate-LE) (Figure 7) (60) is an ester corticosteroid with a high therapeutic index, containing an ester rather than a ketone, at carbon-20 of the prednisolone core structure. LE is indicated for the treatment of steroid responsive inflammatory conditions associated to the palpebral and bulbar conjunctiva, cornea, and anterior segment of the globe. Its mechanism of action is to block the inflammatory mediators treating the inflammation associated with the dry eye disease. Cyclosporine A as already mentioned above is a standard molecule against inflammation with efficacy in dry eye disease, enhancing or restoring the lachrymal gland secretion in patients suffering from this syndrome (61). An advantage of topical loteprednol pretreatment is the reduction of Cyclosporine stinging in chronic dry eye disease (62). Lotemax ophthalmic suspension, 0.5% completed Phase II studies (ClinicalTrials.gov Identifier: NCT00560638) in July 2011. From the results it was confirmed its ability to reduce the eye inflammation rapidly, causing limited side effects. Additionally in 2012 Wan and colleagues performed a study on 34 patients, confirming the efficacy of topical 0.5% loteprednoletabonate ophthalmic suspension for the treatment of moderate dry eye (63).
Ecabet-Sodium
Bausch & Lomb Inc. is developing a prescription eye drop for the treatment of dry eye syndrome called Ecabet (Accession Number: DB05265). Sulfodehydroabietic acid monosodium salt pentahydrate or ecabet sodium, represents a new class of small diffusible molecules capable of increasing the quantity and quality of mucin produced by conjunctival goblet cells and corneal epithelia (Figure 8) (64). This ability makes the compound quite interesting as a treatment for muco-deficient dry eye. Ecabet possible mechanism of action is through the targeting of the prostaglandin E2 pathway, inhibiting the pepsin formation, increasing blood flow and downregulating the reactive oxygen species on the ocular surface. (65). It is marketed in Japan by Senju Pharmaceutical as an oral agent for gastric ulcers and gastritis treatment (66). Bausch & Lomb organized from April 2008 to January 2013 Phase II efficacy and safety studies for Ecabet ophthalmic solution with the purpose of treating the dry eye syndrome (ClinicalTrials.gov Identifier: NCT00667004) in 183 patients. Bausch & Lomb Inc. did not yet distribute results information.
BOL-303242-X
Pharmaceutical R&D, Bausch & Lomb Inc., presented the drug BOL-303242-X (mapracorat) (Figure 9) a selective glucocorticoid receptor agonist, as a possible treatment for inflammatory skin and eye diseases. This agonist is binding to the glucocorticoid receptor with an affinity similar to dexamethasone. Zhang and colleagues demonstrated during in vitro and in vivo studies that BOL-303242-X inhibited interleukin-1b (IL-1b) and induced decreases of inflammation in human corneal epithelial cells. It is possible that BOL-303242-X is acting as an anti-inflammatory agent in various primary human ocular cells with similar activity to classical steroids. As mechanism of action it is suggested its interference in human ocular cells MAPK (p38 and JNK) and NFkB signaling pathways (67). Vollmer T.R. and colleagues confirmed that mapracorat exerts its anti-inflammatory effects, at least in part, by augmenting MAPK phosphatase-1 (MKP-1) expression (68). The compound has an improved side-effect profile, compared to classical glucocorticoids. On the other hand farther research is necessary due to reports of skin atrophy produced in some patients (69). Bausch & Lomb performed Phase II studies on 350 patients, to assess the safety and efficacy of 0.3%, 2% BOL-303242-X in dry eye syndrome, (ClinicalTrials.gov Identifier: NCT01163643) from July 2010 to November 2012 but did not publish results.
AL43546
AL43546 is an ophthalmic solution developed by Alcon. It is consisted of hydroxypropyl guar galactomannan 0.15% or 0.25% (Figure 10). Guar galactomannan is used to add viscosity to artificial tears. In September 2008 Alcon started a Phase II clinical pharmacological study of AL-43546 ophthalmic compound in subjects with shortened tear film break up time, to study the lacrimal fluid condition chronologically after a single dose of AL-43546 ophthalmic solution (ClinicalTrials.gov Identifier: NCT00760045) (70). The results were not published.
Sirolimus-Rapamycin
Sirolimus is an antibiotic demonstrating immunosuppressive and anti-inflammatory properties. Its mechanism of action is to block T-cell activation and proliferation, to activate p70 S6 kinase and to inhibit significantly the production of Th1 cytokines (IFN γ, IL-2 and TNF) (71). Its name is derived from a native word from Easter Island, Rapi Nui (Figure 11). Santen Pharmaceutical is working with subconjunctival injections of sirolimus as a mTOR inhibitor to treat dry eye (72). It is reported that the activation of rapamycinmTOR signaling mediates nerve growth factor (NGF) inducing cell migration (73). From December 2008 to July 2010, Santen realized a Phase II dose-ranging clinical study (ClinicalTrials.gov Identifier: NCT00814944) to assess the safety and efficacy of subconjunctival injection of sirolimus on 143 patients with dry eye in a controlled adverse environmental (CAE) model. The doses applied were 220, 440 and 880 micrograms of rapamycin. The results indicated that sirolimus is safe and tolerable with no systemic adverse events noted, demonstrating bioactivity as immunomodulatory and corticosteroid-sparing agent. It is proved capable to reduce vitreous haze and cells, improving visual acuity (74).
ISV-101
ISV-101 is a new drug of the company InSite Vision incorporating a low dose of the non-steroidal anti-inflammatory (NSAID) bromfenac (Figure 12) and a flow-able mucoadhesive polymer of DuraSite technology (75). This combination enables a slow release of bromfenac over a longer period of time. Consequently the eye aqueous humor is absorbing and retains a higher dose of bromfenac. The extension of the duration of drug residence on the surface of the eye enables better penetration, improving efficacy, safety and dosing. Initial data from previous clinical studies evaluating this combination demonstrated a favorable safety profile. The company started Phase II clinical trials (ClinicalTrials.gov Identifier: NCT01478555) in July 2012 on 150 patients to evaluate the safety, tolerability, and efficacy in topical administration of different dose regimens of the ISV-101.
ESBA-105
ESBATechdeveloped ESBA-105 a single-chain antibody fragment that targets tumor necrosis factor alpha (TNF-a) (76). Selective inhibition of TNF-a has the potential of modulating the inflammatory and immune response. Preclinical studies demonstrated that topically administered ESBA105 attains therapeutic levels in both the anterior and posterior segments of the eye without a need of a penetration enhancer. Consequently, its drug penetration and ocular bio-distribution appear highly attractive for clinical use to treat TNF-a connected eye diseases (77). Alcon after the fusion with ESBATech conducted Phase II clinical trials (ClinicalTrials.gov Identifier: NCT01338610) in April 2011 up to February 2012 to evaluate the efficacy of ESBA-105 10 mg/mL in 90 patients with severe dry eye experiencing persistent ocular discomfort. The results demonstrated that the compound topically applied penetrated into the anterior chamber of the human eye at therapeutic levels (78).
DA-6034
Dong-A Pharmaceutical Co., Ltd is developing a MMP-9 inhibitor called DA-6034, consisting of 7-carboxymethyloxy-3’,4’,5-trimethoxy flavone monohydrate (Figure 13) as possible treatment for dry eye. DA-6034 is a synthetic derivative of eupatilin, a pharmacologically active flavone, capable to increase secretion of mucin-like glycoprotein. It may increase as well the secretion of some mucin species in conjunctiva and cornea. Mucin is a glycoprotein lubricating component of tear film able to weaken moisture loss from tear evaporation. Choi and colleagues verified that DA-6034 at concentrations above 100 microM increased mucin-like glycoprotein levels in animal models, in conjunctival and corneal epithelial cells (79). Furthermore in human conjunctival epithelial cells, DA-6034 treatment in doses of 200 microM increased mucin secretion between the trans-membrane mucins MUC1, MUC2, MUC4, MUC5AC, MUC5B, and MUC16 (79). Seo and colleagues investigated the inhibiting effect of DA-6034 MMP-9 on inflammatory cytokines and the activation of the MAPK signaling pathway on rabbit inflammation models. It was demonstrated that DA-6034 could restore tear function and inhibit inflammatory responses reducing the phosphorylation of Jun N-terminal kinase (JNK) and p38 MAPK, inhibiting the nuclear factor kappa B cells (NF-kB) activation in corneal epithelial cells (80). The NF-κB is a key transcription factor pathway, responsible for many key biological processes, such as inflammation, apoptosis, stress response, corneal wound healing, and angiogenesis (81). The company Dong-A started a Phase II study of DA-6034 (ClinicalTrials.gov Identifier: NCT01670357) in January 2012 to determine the efficacy and safety of 3% or 5% DA-6034 eye drops on 150 patients with doses of one drop/each eye, four times/day, for four weeks.
RX-10045
Resolvyx Pharmaceuticals developed RX-10045 (Figure 14) a small lipid mediator as a product candidate for the treatment of ocular surface and anterior segment diseases (82). In 2010 Celtic Therapeutics and Resolvyx Pharmaceuticals started to collaborate in the development of the compound. RX-10045 is a synthetic resolvin E1 (RvE1) analog formulated for topical application treatment of eye disease as a potent mediator of inflammatory resolution, endogenously produced by the human body from omega-3 fatty acid (83). In pre-clinical dry eye models, RX-10045 has demonstrated potent efficacy. The compound successfully completed a Phase II study (ClinicalTrials.gov Identifier: NCT00799552) in dry eye patients and according to the companies it demonstrated significant symptom improvement from baseline (as assessed in subject diaries), and performed significantly better than placebo on the primary endpoint of the worst symptom score with a 75% reduction in controlled adverse environment-induced central corneal staining from baseline (84). RX-10045 was evaluated in another Phase II study (ClinicalTrials.gov Identifier: NCT01675570) from August 2012 to February 2013 on 150 patients for the treatment of dry eye disease but the results are not yet published.
TobraDex
TobraDex was approved by FDA as dry eye treatment in 1988. TobraDex is a combination of tobramycin and dexamethasone (Figure 15). Tobramycin is an aminoglycoside antibiotic-antibacterial derived from streptomycestenebrarius and is used to treat various types of eye infections. It is working through binding to a site on the bacterial 30S and 50S ribosome, preventing formation of the 70S complex, inhibiting mRNA to be translated into protein (85). Dexamethasone is a potent synthetic member of the glucocorticoid class of steroid drugs used to reduce the inflammation and relieve the symptoms of the inflammatory eye (86). The combination of tobramycin/dexamethasone might be an interesting solution for dry eye problems caused by inflammation and infection. Lately Alcon is evaluating a reformulation of TobraDex decreasing the amount of the steroid (from 0.1% to 0.05%) adding an inactive agent (xanthan gum), to stabilize the combination and to deliver more of each drug to the eye. The composition provides longer ocular retention for enhanced ocular bioavailability of tobramycin and dexamethasone and improved suspension of dexamethasone (87). Alcon executed Phase III clinical trials (ClinicalTrials.gov Identifier: NCT00576251) in June 2007 for TobraDex ophthalmic suspension, containing 0.3% of tobramycin and 0.05% and now is marketing the product as an antibiotic to treat bacterial infections.
SYL1001
The Spanish biotechnology company Sylentis is developing the compound SYL1001, which is decreasing the pain related to dry eye disease, is acting by targeting the TRPV1gene expression on the ocular surface (interference RNA, RNAi) (84, 85). This is an interesting approach as gene silencing is an attractive aspect avoiding the activity of some proteins by inhibiting its synthesis. In November 2010 Sylentis started a Phase II safety/efficacy study (ClinicalTrials.gov Identifier: NCT01776658) on patients with common mild to moderate dry eye symptoms and persistent daily symptoms for more than three months. The study is still ongoing but the initial results are very promising.
R932348
Rigel Pharmaceuticals is working on R932348 2,4-pyrimidinediamine, a small JAK3 molecule inhibitor, as a possible treatment for autoimmune diseases (Figure 16) (88). During trials it was observed that systemic levels of IL-17, IL-22, IL-23, and TNF-a were significantly lower in mice receiving the compound, and T cells isolated from R932348-treated mice also showed reduced phosphorylation of Stat5 after stimulation with IL-2 (89). The company in July 2013, started Phase II safety, tolerability and pharmacokinetics studies (ClinicalTrials.gov Identifier: NCT01900249) for 0.2% and 0.5% R932348 ophthalmic solution in patients with dry eye disease.
EBI-005
Eleven Biotherapeutics is developing chimeric IL-1 receptor type I agonists and antagonists as dry eye treatment. These non-naturally occurring cytokine domains can modulate cellular signaling response to interleukin-1 receptor I (IL-1 RI), and to detect and or even bind on cellular receptors(90). The drug started in December 2012 Phase I multi-center clinical trials (ClinicalTrials.gov Identifier: NCT01745887) with the name EBI-005-2, an IL-1 receptor blocker, single-domain protein, optimized for topical ocular delivery. The EBI-005 has been validated in clinical proof-of-concept studies in which IL-1 blockage was shown to be safe and well tolerated without adverse side effects. According to the results presented in ARVO 2012 (91) it was created by combining the IL-1 receptor binding the sub-domains IL-1β and IL-1Ra. During the pre-clinical trials EBI-005 was shown more active than topical Cyclosporine (the active ingredient of Restasis™ ophthalmic emulsion eye drops) in mouse models. Topical delivery resulted in distribution to multiple eye compartments, but very low systemic exposure in rabbits (F < 0.2%). EBI-005 was 9°C more thermally stable than anakinra an interleukin-1 receptor antagonist (92). Eleven Biotherapeutics presented promising preliminary clinical data from the trials.
Concluding remarks
Many of the above mentioned potential drugs are anti-inflammatory compounds and some are mucin secretagogue, promoting mucin and water production, and also there are a few eye lubricants. Most of the anti-inflammatories are corticosteroids because of their noteworthy anti-inflammatory properties and rapid action. Normally they are used for a limited period of time and depending on the severity of the case, after treatment the patient returns to the initial inflammatory condition. This limitation makes them unsuitable for chronic dry eye therapy as steroidal compounds present important side effects, such as increase in intraocular pressure and posterior sub-capsular cataract (93). A critical point to highlight is that all of the above-mentioned potential new drugs are centering their action mainly towards symptoms, controlling inflammation or restoring the normal amount of tears but none of them is addressing the causative mechanisms of the disease leaving its cause unattended. Developing a new drug for the treatment of DED has become a key target for the pharmaceutical industry. Even though dry eye is the most widespread eye disorder, there is limited offer of effective therapeutic agents. Dry eye disease is not a life-threatening disorder and its symptoms are not severe, but the overarching complexity of the syndrome makes it challenging to manage. Many of the candidate dry eye agents are failing FDA testing, even though some of them are approved in Asia and Europe, mainly because of the tight clinical trials regulations in the USA. Other reasons for this frequent failure are the nature of the syndrome and the lack of an objective test for the diagnosis of the severity of the disease, because usually symptoms evaluation is insufficient as a measurement factor. There are several proposals for new, objective tests such as molecular markers (94, 95) and tear film osmolarity tests (96, 97) but at the moment none of them has advanced beyond the pre-clinical evaluation. Dozens of companies have placed under development a vast variety of new drug candidates in their pharmaceutical pipelines and most of these drugs have already approved as treatment for other diseases as identical biological pathways can be active in different ways in various diseases. Discovering new uses for old drugs can ensure important financial benefits, for patients as well as for biotechnology companies, lowering costs and shortening the approval timelines.
Acknowledgments
We would like to thank the Spanish Ministry of Economy and Competition (Project SAF2010-16024) and the Ministry of Health Social Services and Equality (Project RETICS RD12/0034/0003) for their funding contribution to this publication.
Drug |
Company |
Properties |
Phase |
AL-2178/Rimexolone |
Alcon/Novartis |
Anti-inflammatory |
Phase III |
LX214/Voclosporin |
Isotechnika and Lux Biosciences |
Anti-inflammatory |
Phase I |
Tofacitinib |
Pfizer Inc. |
Anti-inflammatory |
Phase II |
Nutrilarm®-Omega-3 and Omega 6 fatty acids |
ThéaLaboratoire |
Anti-inflammatory |
Phase II |
Omega-3-acid ethyl esters |
Lovaza, GlaxoSmithKline |
Anti-inflammatory |
Phase I |
Secukinumab and Canakinumab |
Novartis Pharmaceuticals |
Anti-inflammatory |
Phase II |
MIM-D3 |
Mimetogen Pharmaceuticals |
Mucin secretagogue |
Phase II |
Difluprednate-Durezol |
Alcon/Novartis |
Anti-inflammatory |
Phase II |
Cis-urocanic acid |
LaurantisPharma |
Anti-inflammatory |
Phase I |
Thymosin Beta 4 |
RegeneRx Biopharmaceuticals, Inc. |
Anti-inflammatory |
Phase II |
Belimumab |
University of Udine |
Anti-inflammatory |
Phase II |
Rituximab |
IDEC Pharmaceuticals |
Anti-inflammatory |
Phase III |
Lotemax |
Bausch & Lomb Inc. |
Anti-inflammatory |
Phase II |
Ecabet sodium |
Bausch & Lomb Inc. |
Mucin secretagogue |
Phase II |
BOL-303242-X (mapracorat) |
Bausch & Lomb Inc. |
Anti-inflammatory |
Phase II |
AL43546 |
Alcon/Novartis |
Artificial tears |
Phase II |
Sirolimus-Rapamycin |
Santen Pharmaceutical |
Anti-inflammatory and immunosuppressive |
Phase II |
ISV-101 |
InSite Vision |
Anti-inflammatory |
Phase II |
ESBA-105 |
Alcon and ESBATech |
Anti-inflammatory |
Phase II |
DA-6034 |
Dong-A Pharmaceutical Co. |
Mucin secretagogue |
Phase II |
RX-10045 |
Resolvyx Pharmaceuticals |
Anti-inflammatory |
Phase II |
Tobradex (tobramycin/ dexamethasone) |
Alcon/Novartis |
Anti-inflammatory |
Phase I |
SYL1001 |
Sylentis |
Lowers dry-eye related pain |
Phase II |
R932348 |
Rigel Pharmaceuticals |
Anti-inflammatory |
Phase II |
EBI-005 |
Eleven Biotherapeutics |
Anti-inflammatory |
Phase I |
Table 1.- Drugs and properties.
Table 2.- Drug Chemical Structures.
Drug |
Chemical structure |
|
Fig. 2 |
AL-2178/ Rimexolone |
Ver PDF |
Fig. 3 |
LX214/ Voclosporin |
|
Fig. 4 |
Tofacitinib |
|
Fig. 5 |
MIM-D3 |
|
Fig. 6 |
Difluprednate-Durezol |
|
Fig. 7 |
Lotemax |
|
Fig. 8 |
Ecabet sodium |
|
Fig. 9 |
BOL-303242-X (mapracorat) |
|
Fig. 10 |
AL43546/ galactomannan |
|
Fig. 11 |
Sirolimus |
|
Fig. 12 |
ISV101/ bromfenac |
|
Fig. 13 |
DA-6034 |
|
Fig. 14 |
RX-10045 |
|
Fig. 15 |
Tobradex (tobramycin/ dexamethasone) |
|
Fig. 16 |
R932348 |
REFERENCeS
3. Abusharha AA, Pearce EI. The Effect of Low Humidity on the Human Tear Film. Cornea. (2012).
8. Dilly PN. Structure and function of the tear film. Adv Exp Med Biol. 350 239-47 (1994).
11. Lemp MA. Epidemiology and classification of dry eye. Adv Exp Med Biol. 438 791-803 (1998).
26. AL-2178. ClinicalTrials.gov Identifier: NCT00471419 http://clinicaltrials.gov/ct2/show/NCT00471419?term=AL-2178+Rimexolone&rank=1. (2008).
28. LX214. ClinicalTrials.gov Identifier: NCT00851734 http://clinicaltrials.gov/ct2/show/NCT00851734?term=LX214&rank=1. (2012).
40. Dhimolea E. Canakinumab. MAbs. 2(1), 3-13 (2010).
47. Boltralik JJ. Anti-inflammatory compounds for ophthalmic use. US19955446177 (1995)
51. Sosne G, Crockford D. Methods and compositions for stabilizing polypeptides. WO2008108927 (2008)
56. Belimumab. ClinicalTrials.gov Identifier: NCT01160666 http://clinicaltrials.gov/ct2/show/NCT01160666?term=Belimumab+Sjogren&rank=1. (2012).
58. Rituximab. ClinicalTrials.gov Identifier: NCT00740948 http://clinicaltrials.gov/ct2/show/NCT00740948?term=Rituximab+Sjogren&rank=1. (2013).
60. Bartels PS. Use of loteprednol etabonate for the treatment of dry eye. WO2005094836A2 (2005)
70. AL-43546. ClinicalTrials.gov Identifier: NCT00760045 http://clinicaltrials.gov/ct2/show/NCT00760045?term=AL43546&rank=1. (2010).
76. Urech DM. Functionalized polypeptides. WO2010006454 (2010)
83. Therapeutics C. Developing therapies for critical unmet medical needs. RX 10045 - Dry Eye and Allergic Conjunctivitis. http://www.celtictherapeutics.com/RX100452012.
84. Pharmaceuticals R. RX-10045 http://www.resolvyx.com/products/rx-10045.asp2013.
88. Wong B. JAK kinase inhibitors and their uses. US20060270694 (2006)
95. Pintor J. (A molecular marker for dry eye). Arch Soc Esp Oftalmol. 82(3), 129-30 (2007).